Expert Treatment & Custom Scleral Lenses in Houston. Trusted by Texans for Over 60 Years
What Is Keratoconus?
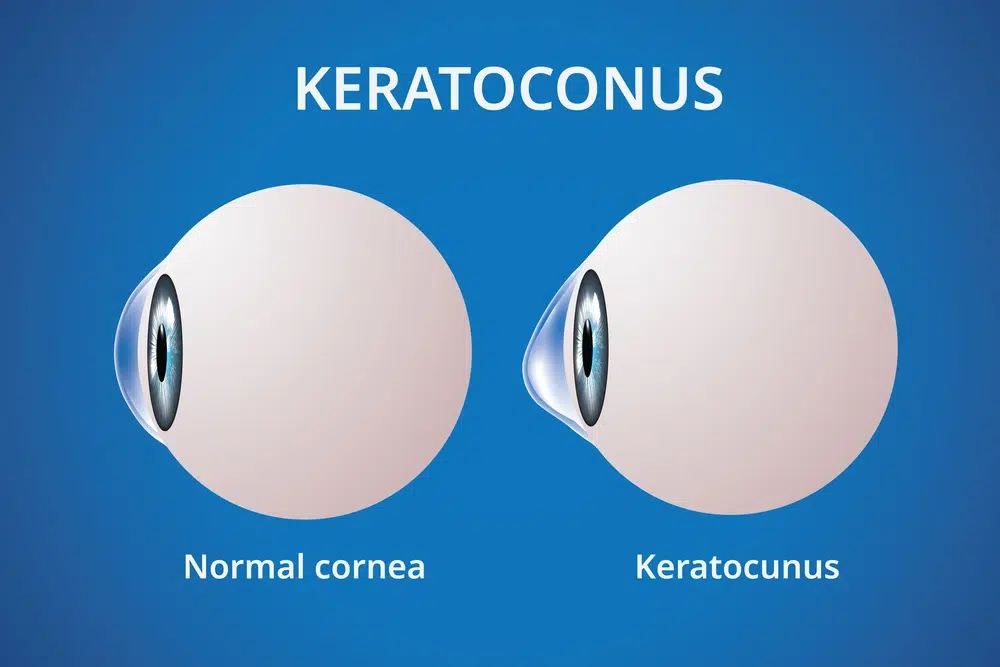
Keratoconus is a progressive eye condition that affects the cornea—the clear, dome-shaped window at the very front of your eye. In a healthy eye, the cornea has a smooth, round shape, like a baseball.
In an eye with keratoconus, the collagen fibers within the cornea weaken. This causes the cornea to gradually thin and bulge outward into an irregular, cone-like shape. Because the cornea is responsible for focusing light into the eye, this distorted “cone” shape scatters the light, resulting in severely distorted and blurred vision that cannot typically be corrected with standard glasses or soft contact lenses.
On This Page
Signs and Visual Symptoms
Keratoconus typically begins to develop in a person’s teenage years or early twenties and can slowly progress for 10 to 20 years before stabilizing. The rate of progression varies greatly from patient to patient.
Common symptoms include:
- Blurry, distorted, or “wavy” vision.
- Increased sensitivity to bright light and glare.
- Seeing “halos” or “starbursts” around lights, especially at night.
- A rapidly changing eyeglass or contact lens prescription.
- Difficulty driving at night.
Essentially, RLE leverages the advanced lens technology used in cataract surgery to proactively correct vision before cataracts become visually significant.

Causes and Risk Factors
While the exact cause of keratoconus is still being researched, clinical studies suggest it is tied to a combination of genetic, environmental, and cellular factors.
- Eye Rubbing (The #1 Modifiable Risk): Vigorous, chronic eye rubbing is heavily linked to the development and rapid progression of keratoconus.
- Genetics: A family history of keratoconus increases your risk.
- Allergies: Conditions like hay fever, eczema, and asthma are frequently seen in keratoconus patients, primarily because they lead to chronic itchy eyes and, consequently, eye rubbing.
Advanced Diagnosis at Berkeley Eye Center
Early detection is the most crucial factor in effectively managing keratoconus. Because early-stage keratoconus mimics standard astigmatism, specialized technology is required for an accurate diagnosis. Our Houston specialists utilize state-of-the-art imaging:
- Corneal Topography: This non-invasive, painless imaging technique creates a highly detailed, 3D topographical map of your cornea’s surface curvature. It allows our doctors to detect the microscopic, early signs of a developing cone long before symptoms become severe.
- Pachymetry: This specialized test measures the exact thickness of your cornea, which is vital for diagnosing the thinning associated with keratoconus and monitoring its progression over time.
Is Scleral Lens Treatment Right for You?
You may be an excellent candidate for life-changing scleral lens treatment if you:
The only way to know for certain is through a comprehensive evaluation with our keratoconus specialists. We’ll perform advanced corneal mapping and often let you try diagnostic scleral lenses during your visit so you can experience the visual difference immediately.
Keratoconus Treatment Options: Restoring Your Vision
A keratoconus diagnosis does not mean you have to settle for poor vision. While there is no cure, we have incredibly effective ways to manage the condition and restore your sight.
Because standard glasses and soft contacts sit poorly on a cone-shaped eye, custom specialty contact lenses are the gold standard for keratoconus visual rehabilitation.
The Life-Changing Power of Scleral Lenses
Not all lenses are created equal. For moderate to advanced keratoconus, Scleral Lenses are widely considered the absolute best treatment option.
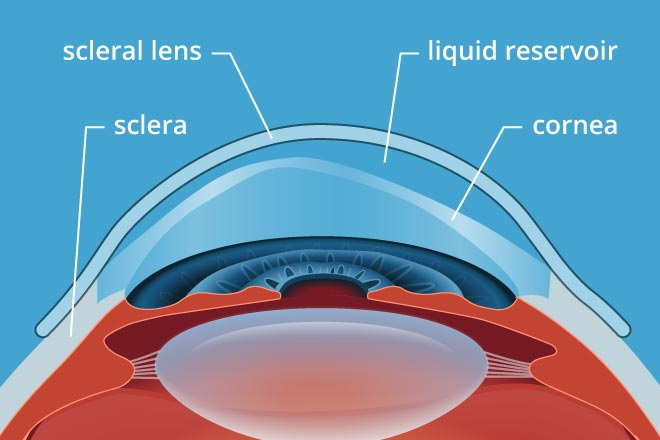
These large-diameter, rigid gas-permeable lenses are custom-designed to vault completely over the irregular, cone-shaped cornea and rest gently on the white part of the eye (the sclera). This creates a gap between the lens and the cornea that is filled with soothing saline. The liquid reservoir masks the irregular cornea underneath, essentially creating a perfectly smooth, brand-new optical surface. The result is crisp, clear vision and phenomenal comfort.
Other Specialty Lens Options
Depending on the stage of your condition, our doctors may also recommend:
Our specialty lens fitters will work closely with you, utilizing trial lenses during your evaluation so you can experience the visual difference firsthand!
What Vision Results Can You Expect?
Clinical outcomes for keratoconus patients fitted with specialty contact lenses are exceptional:
Your individual results depend on the severity of your keratoconus, corneal scarring (if present), and how well the lenses are fitted to your unique eye shape.

Lifestyle Tips for Managing Keratoconus
Alongside professional medical care, you can take active steps to protect your corneas:
Frequently Asked Questions About Keratoconus
Will keratoconus make me go blind?
No. While keratoconus can cause significant visual impairment and make daily tasks difficult if left untreated, it does not cause total blindness. With modern treatments like custom scleral lenses, the vast majority of patients achieve excellent, functional vision and maintain a high quality of life.
Can keratoconus be cured or reversed?
Currently, there is no cure for keratoconus, and the thinning of the cornea cannot be reversed. However, the progression of the disease naturally slows down and usually halts by the time a patient reaches their 30s or 40s. Our goal is to manage your vision effectively throughout your life.
Why are scleral lenses better than glasses for keratoconus?
Glasses sit far away from the eye and can only correct basic refractive errors. They cannot compensate for the irregular, bumpy, cone-like surface of a keratoconic cornea. Scleral lenses vault over this irregularity, and the fluid reservoir underneath the lens neutralizes the distortion, providing vastly superior visual clarity.
Will I eventually need a corneal transplant?
Decades ago, corneal transplants were common for advanced keratoconus. Today, thanks to the incredible advancements in specialty contact lenses (like sclerals), the need for corneal transplant surgery has decreased dramatically. A transplant is now considered a last resort when a patient can no longer tolerate or achieve good vision with specialty lenses.
What is the difference between scleral lenses and regular RGP lenses for keratoconus?
Both are rigid gas permeable lenses that can correct keratoconus, but scleral lenses are much larger (14-24mm vs 9-10mm diameter) and vault completely over the cornea to rest on the white of the eye, creating a fluid reservoir underneath. This makes sclerals significantly more comfortable than traditional RGPs and provides more stable vision for moderate to advanced keratoconus. Traditional RGPs sit on the cornea and can be uncomfortable or pop out easily on an irregular surface. Most keratoconus specialists now prefer scleral lenses for better outcomes and patient satisfaction.
Can I drive at night with keratoconus?
Untreated keratoconus makes night driving extremely difficult or impossible due to severe halos, starbursts, and glare from headlights and street lights. With properly fitted scleral lenses, the vast majority of our keratoconus patients regain the ability to drive safely at night. The clear, crisp vision provided by sclerals eliminates the distortion and allows you to see clearly in all lighting conditions.
How long does it take to get fitted for scleral lenses?
The fitting process typically takes 2-4 appointments over several weeks. We use advanced corneal topography to map your eye’s unique shape, then select diagnostic lenses to evaluate fit and vision. Once we’ve achieved the optimal fit, your custom lenses are ordered. Most patients notice dramatic vision improvement from the very first trial lens.
Why Choose Berkeley Eye Center for Your Keratoconus Treatment
Take Control of Your Keratoconus Today
Don’t let keratoconus dictate your quality of life. At Berkeley Eye Center, we understand the frustration of distorted vision, and we have the advanced technology and customized lens solutions to help.
